Chronic Venous Insufficiency (CVI) is a common vascular condition that occurs when the veins in the legs have difficulty returning blood back to the heart. This condition leads to pooling of blood in the lower extremities, causing swelling, pain, skin changes, and, in severe cases, venous ulcers. CVI is a long-term condition that can significantly affect a person’s quality of life if left untreated.
This article explores the causes, symptoms, stages, diagnosis, prevention, and treatment options for Chronic Venous Insufficiency. We will also discuss lifestyle changes, risk factors, and medical procedures that can help manage or reverse the condition.
Understanding Chronic Venous Insufficiency
Veins are responsible for carrying blood back to the heart. In the legs, this process works against gravity, aided by valves inside the veins that prevent blood from flowing backward. When these valves become weakened or damaged, blood flows backward and collects in the veins. This condition is called venous reflux, which leads to chronic venous insufficiency.
CVI is often associated with varicose veins and deep vein thrombosis (DVT). Over time, the increased pressure inside the veins causes inflammation, pain, and visible changes in the skin.
Causes of Chronic Venous Insufficiency
There are several underlying causes of CVI, many of which involve damage or weakness in the vein walls or valves. The most common causes include:
- Varicose veins: These twisted, enlarged veins result from faulty valves and are one of the main causes of CVI.
- Deep vein thrombosis (DVT): Blood clots in the deep veins can damage valves and obstruct normal blood flow.
- Valve dysfunction: Genetic predisposition or injury can weaken the vein valves, leading to CVI.
- Obesity: Excess body weight increases pressure on the veins in the legs.
- Prolonged standing or sitting: Occupations requiring long hours in one position can hinder proper blood circulation.
- Leg injuries or surgeries: Trauma or operations can damage vein walls or valves.
- Pregnancy: Hormonal changes and increased blood volume during pregnancy can affect the veins, sometimes causing long-term insufficiency.
- Age: As we age, vein walls lose elasticity, and valves become less efficient.
- Genetics: A family history of venous disorders increases the risk of developing CVI.
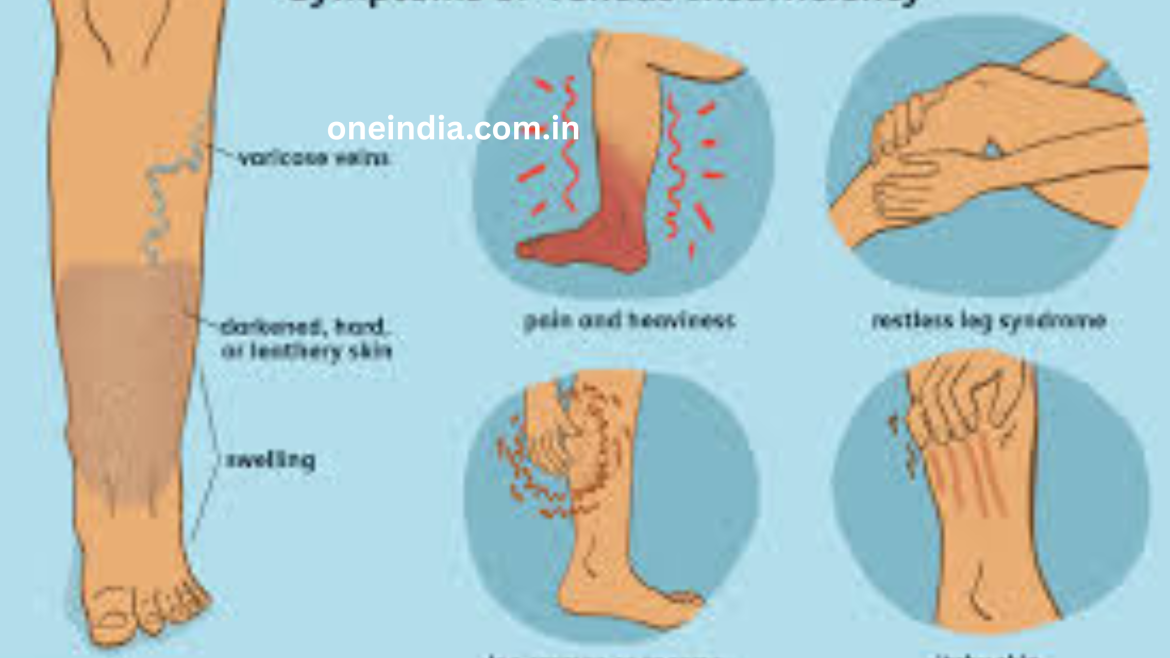
Symptoms of Chronic Venous Insufficiency
The symptoms of CVI vary based on the severity of the condition. In the early stages, symptoms may be mild but worsen over time if left untreated.
Common Symptoms Include:
- Swelling in the ankles, calves, or feet (edema).
- Aching, throbbing, or heavy sensation in the legs.
- Pain that worsens after long periods of standing.
- Skin discoloration, especially around the ankles (brownish or reddish patches).
- Varicose veins or spider veins.
- Itching, flaking, or thickening of the skin.
- Leg cramps, particularly at night.
- Restless legs or tingling sensations.
- Open sores or ulcers on the lower legs, typically near the ankles.
Stages of Chronic Venous Insufficiency
CVI is classified into different stages based on its severity, often referred to as the CEAP classification (Clinical, Etiological, Anatomical, and Pathophysiological):
- C0: No visible or palpable signs of venous disease.
- C1: Presence of spider veins or reticular veins.
- C2: Varicose veins are visible.
- C3: Swelling (edema) in the legs without skin changes.
- C4: Skin changes such as pigmentation or eczema.
- C5: Healed venous ulcers.
- C6: Active venous ulcers.
Understanding the stage of CVI is essential for determining the appropriate treatment strategy.
Risk Factors for CVI
While anyone can develop chronic venous insufficiency, some factors increase the likelihood of developing the condition:
- Family history of venous disorders.
- Older age.
- Being overweight or obese.
- Sedentary lifestyle or lack of physical activity.
- Pregnancy (especially multiple pregnancies).
- Gender (women are more prone due to hormonal factors).
- Prolonged periods of sitting or standing.
- History of deep vein thrombosis or leg injuries.
Complications of Chronic Venous Insufficiency
If untreated, CVI can lead to several complications, including:
- Venous ulcers (open sores that heal slowly).
- Chronic leg pain or swelling.
- Cellulitis (skin infection due to poor circulation).
- Lipodermatosclerosis (thickening and hardening of the skin).
- Bleeding from varicose veins due to fragile skin.
- Deep vein thrombosis in severe cases.
Diagnosis of Chronic Venous Insufficiency
A healthcare professional uses several methods to diagnose CVI, including a detailed medical history, physical examination, and imaging tests.
Common diagnostic procedures include:
- Doppler ultrasound: A non-invasive test that uses sound waves to check blood flow in the veins.
- Duplex ultrasound: Provides detailed images of the veins and evaluates valve function.
- Venography: A contrast dye and X-ray test to visualize blood flow (rarely used now due to advanced ultrasound technology).
- Physical examination: Checking for swelling, varicose veins, skin changes, and ulcers.
Treatment of Chronic Venous Insufficiency
The treatment of CVI focuses on improving blood flow, reducing symptoms, and preventing complications. The choice of treatment depends on the severity of the condition.
Lifestyle Changes and Home Remedies
- Regular exercise to improve blood circulation.
- Elevating legs for 15-20 minutes several times a day.
- Wearing compression stockings to promote blood flow.
- Avoiding prolonged sitting or standing.
- Maintaining a healthy weight to reduce pressure on veins.
- Keeping skin moisturized to prevent dryness and irritation.
Medical Treatments
- Compression therapy: Specialized compression stockings are recommended to prevent blood pooling.
- Medications: Drugs like venoactive agents can reduce pain and swelling.
- Wound care: For venous ulcers, proper dressing and care are essential.
Minimally Invasive Procedures
- Endovenous laser therapy (EVLT): A laser fiber closes the affected vein.
- Radiofrequency ablation (RFA): Uses heat to seal damaged veins.
- Sclerotherapy: A chemical solution is injected to close varicose veins.
- VenaSeal: A medical glue is used to close the vein.
Surgical Treatments
- Vein stripping and ligation: Removing or tying off damaged veins.
- Ambulatory phlebectomy: Removing smaller varicose veins through tiny incisions.
- Bypass surgery: For severe cases when other treatments fail.
Prevention of Chronic Venous Insufficiency
While not all cases of CVI can be prevented, adopting healthy habits can reduce the risk:
- Maintain an active lifestyle with regular walking or cycling.
- Avoid prolonged sitting or standing.
- Keep legs elevated while resting.
- Wear compression stockings if you have a family history of venous disease.
- Maintain a healthy body weight.
- Avoid tight clothing that restricts blood flow.
- Stay hydrated and eat a balanced diet rich in fiber and vitamins.
Living with Chronic Venous Insufficiency
CVI is a chronic condition, but with proper treatment and lifestyle adjustments, patients can manage symptoms effectively. Regular follow-ups with a vascular specialist, adopting a fitness routine, and maintaining good skin care are essential for improving overall quality of life.
Frequently Asked Questions
What is Chronic Venous Insufficiency (CVI)?
Chronic Venous Insufficiency is a long-term condition where the veins in the legs cannot pump blood effectively back to the heart, causing blood to pool in the lower limbs.
How is CVI different from varicose veins?
Varicose veins are swollen, twisted veins caused by faulty valves, while CVI is a more severe condition involving chronic blood pooling and possible complications like ulcers.
What are the early signs of CVI?
Early signs include mild swelling in the ankles or feet, a feeling of heaviness, and visible spider veins or small varicose veins.
Who is at the highest risk of developing CVI?
Individuals who are older, overweight, pregnant, or have a family history of vein problems are at higher risk. People with sedentary jobs are also vulnerable.
Can CVI occur without visible varicose veins?
Yes, some people may have CVI without visible varicose veins, but they may still experience symptoms like swelling, pain, or skin changes.
Is CVI a life-threatening condition?
CVI itself is not life-threatening, but if left untreated, it can lead to serious complications such as venous ulcers or infections.
How is CVI diagnosed?
CVI is diagnosed through a combination of physical examination, Doppler ultrasound, and duplex imaging to evaluate blood flow and valve function.
Can lifestyle changes alone treat CVI?
For mild cases, lifestyle changes like exercising, wearing compression stockings, and elevating the legs may control symptoms but may not completely cure the condition.
What role do compression stockings play in CVI treatment?
Compression stockings improve blood circulation, reduce swelling, and prevent blood pooling in the legs, making them a primary treatment option.
Does CVI always require surgery?
No, surgery or minimally invasive procedures are considered only if lifestyle changes and conservative treatments fail to improve the condition.
How effective is sclerotherapy for CVI?
Sclerotherapy is highly effective for closing small varicose veins, improving symptoms, and preventing further complications.
Conclusion
Chronic Venous Insufficiency (CVI) is a long-term condition that requires timely diagnosis and management to avoid serious complications like venous ulcers. Understanding the causes, symptoms, and treatment options is crucial for both prevention and recovery. With the combination of medical treatments, lifestyle changes, and proper care, individuals can manage CVI and maintain a healthy, active lifestyle.